why we panic
A classic CBT formulation of that panic which is met with in panic disorder - a formulation owed to David Clark - looks like this:
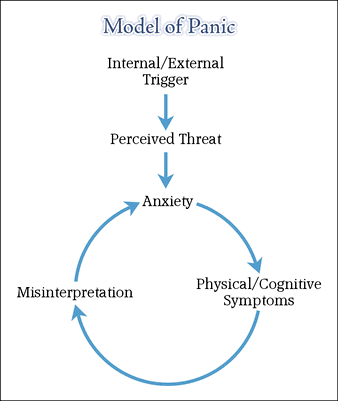
The idea, I believe, is that we're to read the arrows as meaning 'and then this leads to...' We might say that they're perhaps intended as 'causal' relations.
For clinical purposes the model is helpful. The clinician can share the model, and then, with the model now there to help organise a terrifying runaway experience, the patient can start to stand back from her experience too, put it into words, etc. (More on this later.) But does it mean anything to suggest that the model is empirically accurate? How, say, do we know the wheel really spins clockwise rather than anticlockwise? What tests could we run to show that misinterpretations lead to anxiety lead to symptoms, rather than these all being epiphenomenal products of some other underlying circular causal mechanism?
The thing is, I don't think the questions I just asked are actually good questions. My point in asking them is to suggest that if the model is to be understood as it rather invites us to understand it - perhaps in 'mechanistic' terms - then they should be good questions.
 |
| David Clark |
Here's another thing. The value of the cognitive model, as I see it, is that it captures something of our ordinary understanding that panic involves getting in a spin. What the model doesn't explicitly thematise, but what it nevertheless aptly suggests, is that the panicking person has also lost a grounding contact with and in reality, and instead now hyper-reflexively takes what's normally the mere medium of his intentional relatedness to the world (his thoughts, feelings, bodily states, etc.) for its object. (I don't say that by way of offering a causal hypothesis, but instead offer it as a phenomenological articulation of what we already understand.) And we really don't need to think of anxiety as 'leading to' cognitive and physical 'symptoms'. Instead it 'includes' them; they 'constitute' it. And we don't need to think in terms of 'misinterpretation', as if normally we have a different, perhaps saner, interpretation in our minds. Instead what we have is the person becoming involuted, getting in a right state, anxiously worrying that he's having a heart attack or stroke or what have you, and not really being able to think properly any more. What the model misses here is the qualitative character of the state of mind the sufferer is now in: it's a state in which, because healthy exteroceptive reality contact has quite diminished, involves a loss of the capacity to clearly distinguish between fearful fantasies and realities. In the language of Minkowski, this mind has 'short-circuited'.
 |
| Viktor Frankl |
In many ways, as I acknowledged in the second paragraph, none of this matters. It doesn't matter if the model doesn't quite pass muster. It doesn't matter if it inclines somewhat towards the pervily boxological and inhumanly scientistic offerings of the 'cognitive sciences'. It's at the least part of a techne of care, a way to help restore inner order. All that I really want to take a stand against here is the impression it might give us, and which I think it often does give us - that the kind of knowledge that really matters, to help the patient, is of a scientific or quasi-scientific or largely reflective sort. When really that's not the thing at all. What really matters - it seems to me - is the therapist's 'containing' and 'mentalising' function, and their natty pictures take their place in supporting the occurrence of this. (Again, I'm not offering these as empirical claims, but just as ways of describing what we all already know once we clear out the misleading causal claims and just try to describe the situation honestly.) It's their know-how, which is ultimately not something other than their very humanity, which is in play. Can they make themselves truly available for the patient, here, as a receptive mind, one that wants to understand the patient in his own terms, yet one which also brings an additional grasp of our possible human predicaments to bear upon the patient's experience? That's the question.
-----------
Just a quick postscript for trainees. I remember being so struck by the cognitive panic disorder model when training that I somehow thought that it was a model of all panic. But it's really not. People often panic - in a more one-off fashion, rather than in the panic disorder manner, either when the defences against unconscious anxieties break down, or when anxieties bubble over as the severe strains of life aren't adequately 'mentalised'.

Comments
Post a Comment
Comment here!